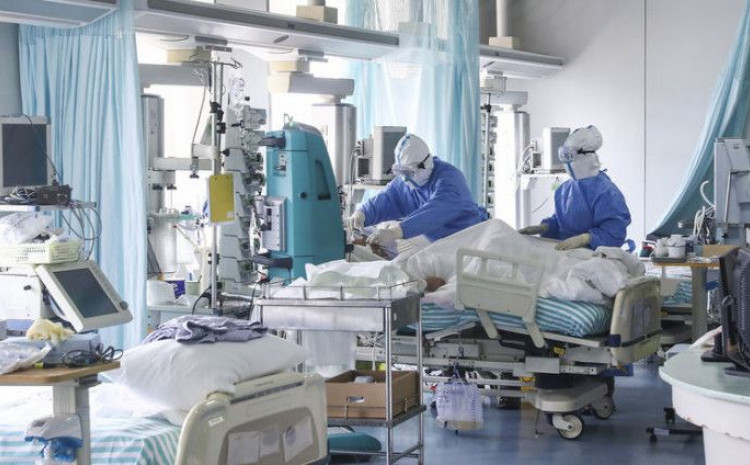
The COVID-19 pandemic has dealt a heavy blow to key health services in Africa, raising worries that some of the continent’s major health challenges could worsen.
The preliminary analysis by the World Health Organization (WHO) of five key essential health service indicators that include outpatient consultation, inpatient admission, skilled birth attendance, treatment of confirmed malaria cases and provision of the combination pentavalent vaccine in 14 countries finds a sharp decline in these services between January and September 2020 compared with the two previous years. The gaps were the widest in May, June and July, corresponding to when many countries had put in place and enforced movement restrictions and other social and public health measures to check the spread of COVID-19. During these three months, services in the five monitored areas dropped on average by more than 50% in the 14 countries compared with the same period in 2019.
“The COVID-19 pandemic has brought hidden, dangerous knock-on effects for health in Africa. With health resources focused heavily on COVID-19, as well as fear and restrictions on people’s daily lives, vulnerable populations face a rising risk of falling through the cracks,” said Dr Matshidiso Moeti, WHO Regional Director for Africa.
“We must reinforce our health systems to better withstand future shocks. A strong health system is the bedrock for emergency preparedness and response. As countries ease COVID-19 restrictions, we must not leave the door open for the pandemic to resurge,” said Dr Moeti. “A new wave of COVID-19 infections could further disrupt life-saving health services, which are only now recovering from the initial impact.”
Even prior to the COVID-19 pandemic, maternal mortality in sub-Saharan Africa was unacceptably high, accounting for about two-thirds of global maternal deaths in 2017. Preliminary data indicates that COVID-19 is likely to exacerbate women’s health challenges and the new analysis found that skilled birth attendance in the 14 countries dropped. In Nigeria, 362 700 pregnant women missed ante-natal care between March and August 2020. Over 97 000 women gave birth away from health facilities and over 193 000 missed postnatal care within two days of giving birth. There were 310 maternal deaths in Nigerian health facilities in August 2020, nearly double the figure in August 2019.
An additional 1.37 million children across the African region missed the Bacille Calmette-Guerin (BCG) vaccine which protects against Tuberculosis (TB) and an extra 1.32 million children aged under one year missed their first dose of measles vaccine between January and August 2020, when compared with the same period in 2019.
Immunization campaigns covering measles, yellow fever, polio and other diseases have been postponed in at least 15 African countries this year. The introduction of new vaccines has been halted and several countries have reported running out of vaccine stocks.
“Now that countries are easing their restrictions, it’s critical that they implement catch-up vaccination campaigns quickly,” said Dr Moeti. “The longer, large numbers of children remain unprotected against measles and other childhood diseases, the more likely we could see deadly outbreaks flaring up and claiming more lives than COVID-19.”
WHO has issued guidance on how to provide safe immunization services, including how to conduct a careful risk assessment before implementing preventive mass vaccination, with attention to appropriate protective measures to avoid transmission of COVID-19. The Central African Republic, the Democratic Republic of the Congo and Ethiopia have already carried out catch up measles vaccination campaigns. Thirteen other African countries aim to restart immunization campaigns for measles, polio and human papillomavirus in the coming months and WHO is providing guidance on COVID-19 prevention measures to keep health workers and communities safe.
WHO has also provided guidance to countries on how to ensure the continuity of other essential health services by optimizing service delivery settings, redistributing health work force capacity and proposing ways to ensure uninterrupted supply of medicine and other health commodities.
As part of the COVID-19 response, health workers have received capacity building in infection, prevention and control, laboratories have been strengthened and data collection and analysis improved. These efforts support the fight against the virus while also building up health systems.
Dr Moeti spoke during a virtual press conference today facilitated by APO Group. She was joined by Professor Ifedayo Adetifa, Clinical Epidemiologist, KEMRI-Wellcome Trust Research Programme and Associate Professor, London School of Hygiene and Tropical Medicine; and Regina Kamoga, Executive Director, Community Health and Information Network and Chairperson of the Uganda Alliance of Patients Organisations.